Eyelid Cancer Reconstruction in St. Louis, MO
What is Eyelid Cancer Reconstruction?
When skin cancer affects the delicate structures around your eyes, experience matters. At Ophthalmic Plastic & Cosmetic Surgery, eyelid cancer reconstruction is performed by fellowship-trained oculofacial plastic surgeons with decades of specialized experience.
Led by Dr. John B. Holds – an award-winning, nationally recognized expert – our team focuses on preserving vision, restoring eyelid function, and achieving natural-looking results.
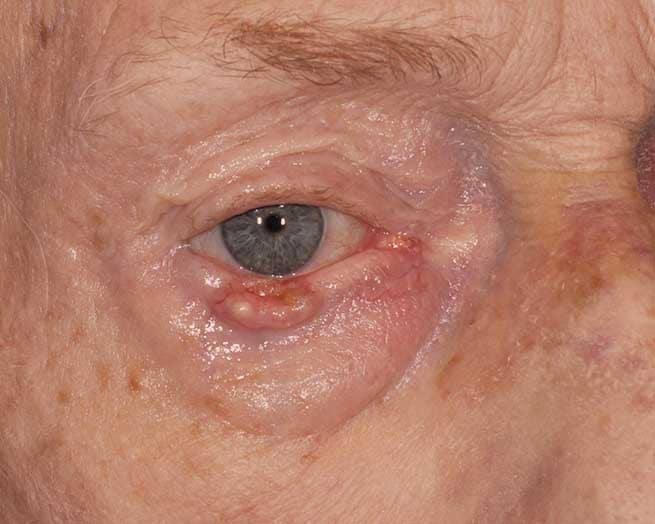
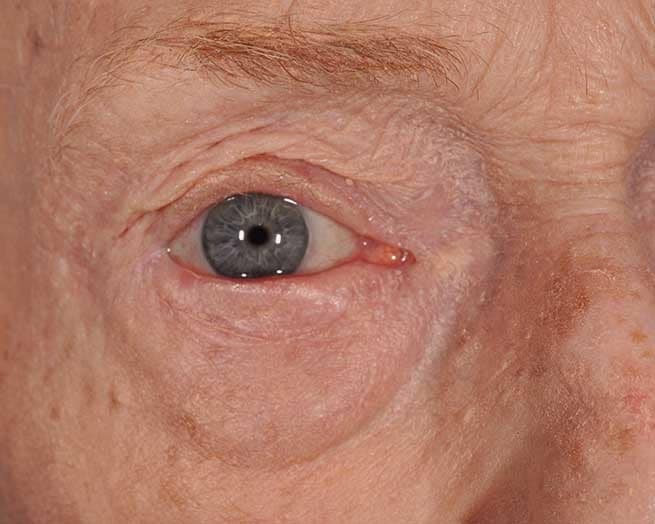
Eyelid Cancer Reconstruction Before and After
Because the eyelids are exposed to the sun all the time, they are particularly susceptible to the development of skin cancer. The following are types of skin cancer that can affect the eyelids.
Basal Cell Carcinoma
Eight out of every 10 skin cancers are basal cell carcinomas, making this form of skin cancer the most common. They grow in the lowest layer of the epidermis, the basal cell layer. These cancers usually develop on sun-exposed areas, especially the head and neck. They tend to grow slowly, and it is rare for them to spread to other parts of the body. If left untreated, basal cell carcinomas can grow into nearby areas and invade bone or other tissues beneath the skin, making removal potentially disfiguring.
Squamous Cell Carcinoma
Squamous cell carcinoma is the second most common form of skin cancer. It forms in the squamous cells that make up the middle and outer layer of the skin. Most squamous cell carcinomas result from prolonged exposure to ultraviolet radiation from the sun, tanning beds, or lamps. Unlike basal cell carcinomas, squamous cell carcinomas can occur in a wider range of locations. Although more common on the sun-exposed skin on the backs of the hands, the ears, the scalp, and the lips, this form of skin cancer can occur anywhere on the body, including inside the mouth and on the genitals. Not considering life-threatening conditions, if treated early, like basal cell carcinoma, it can also be disfiguring. If it spreads, it can be life-threatening.
Melanoma
Most people assume there is just “melanoma.” There are actually four different types of this most dangerous form of skin cancer:
- Superficial spreading melanoma: This is the most common form. It can arise in an existing mole or appear as a new lesion. When it forms in a mole already on the skin, it tends to grow on the surface for a period of time before penetrating more deeply. It is most likely to occur on the torso in men, the legs in women, and the upper back in both sexes. Superficial spreading melanoma appears as flat or slightly raised, discolored patches with asymmetrical borders.
- Lentigo maligna: This form of melanoma often develops in older people. It also grows close to the surface of the skin in the beginning. This form typically develops on sun-damaged areas of the face, ears, arms, and upper torso. Lentigo maligna appears as flat or slightly raised, blotchy patches with uneven borders.
- Acral lentiginous melanoma: This is the most common form of melanoma found in people with darker skin tones, including those with African ancestry. It often forms in areas that are not easy to spot — under the fingernails or toenails, on the soles of the feet, or on the palms of the hands. It appears as a black or brown area.
- Nodular melanoma: This is the most aggressive type of melanoma. It makes up 10-15 percent of all cases. These tumors grow deeper into the skin more rapidly than other types of melanoma. They are invasive tumors, meaning they’re likely to have already reached the deeper layer of skin by the time they are diagnosed. These are found most frequently on the torso, legs, and arms, and on the scalp in older men. These appear as bumps on the skin, typically blue-black in color.
Sebaceous Cell Carcinoma
Sebaceous cell carcinoma is much rarer than the cancers listed above, but it is particularly common in the eyelids. This form of skin cancer begins in an oil gland (a sebaceous gland) in your skin. Sebaceous cell carcinoma may begin as a painless lump or thickening of the skin on the eyelid. As it grows, the cancer may bleed or ooze. Although rare, sebaceous cell carcinoma is more aggressive, as it can spread to other areas of the body.
What our patients have to say
“I’ve been seeing Dr Holds for 28 years by far the best doctor I’ve come across and would highly recommend him to anyone looking for eye surgery or plastic surgery” -Rod C.
“Dr. Holds and his staff are the best. I would highly recommend them. They insure you are happy with anything they do. They produce great results.” Patti H.
A risk factor increases your chances of developing cancer. While risk factors themselves do not cause cancer, if you have any of these, you should see your dermatologist regularly so they can monitor any suspicious lesions on your skin, including your eyelids. Risk factors for developing eyelid cancer include:
- Exposure to UV radiation: Sun exposure contributes to the development of all of these skin cancers. People who live in areas with year-round bright sunlight have a higher risk of developing eyelid cancer. This is also true if you’ve been a regular at a tanning parlor.
- Fair skin: Melanin is the skin’s protection mechanism against UV radiation. That’s why our skin darkens after sun exposure: it’s protecting itself. People with less melanin in their skin have less protection. People with light hair and light-colored eyes who have skin that doesn’t tan but instead freckles or burns easily are at higher risk for developing eyelid cancer.
- Gender: White men are developing these cancers at a higher rate.
- Age: Most basal cell and squamous cell carcinomas appear after the age of 50.
- A history of sunburns: All skin cancers develop from repeated, accumulating sun exposure and damage. This is especially true of basal cell, squamous cell, and sebaceous cell carcinomas. Melanoma is often linked to severe, peeling sunburns. Each of those sunburns that occur in a person’s life doubles their chance of developing melanoma later in life. Melanoma, however, is rare in eyelid cancer.
- Previous skin cancer: If you’ve had any form of skin cancer, that places you at a much higher risk for developing another skin cancer. For instance, about 35 to 50 percent of people who are diagnosed with one basal cell carcinoma will develop a new cancer within five years.
What Happens During Eyelid Cancer Reconstruction?
The usual process in treating suspected eyelid cancer is to first obtain a biopsy to establish the diagnosis. This is generally done during an office visit. Once we have a diagnosis, we decide how to treat the problem. We often work with a specialist dermatologist who performs Mohs excision to ensure complete removal of the skin cancer while minimizing the amount of normal tissue removed.
In this situation, you visit the office of the Mohs surgeon on the day of surgery, and they complete the removal of cancer. You then come to our surgery center, where we complete your reconstruction to be as aesthetic and functional as possible.
We sometimes perform the excision in our operating room, monitoring the margins to ensure complete excision with a technique called a “frozen section.” In this case, we can proceed immediately to the reconstruction.
You may have undergone surgery elsewhere that left you with lids that turn outward or inward, or you may no longer have the ability to fully close your eyes. All of these issues, along with others, can be addressed with eyelid reconstruction.
We typically do not perform cosmetic procedures such as blepharoplasty, midface lift, or laser skin resurfacing as part of the initial eyelid cancer reconstruction. Still, we often perform these procedures later for patients who wish to proceed.
Each eyelid cancer reconstruction is unique, but our team is committed to preserving your vision, ensuring your eyelids function properly, and improving the appearance of your eyes.
Unlike cosmetic eyelid surgery, which involves a relatively easy recovery, reconstructive eyelid surgery recovery is more involved. Patients usually need to wear an eye patch for at least the first 24 hours.
Recovery may take up to two weeks for the bruising and inflammation to fully subside. From there, the extent of the procedure will dictate the remainder of your recovery.
During your consultation, your surgeon will discuss the extent of the reconstruction needed and your expected recovery.
Why Choose Ophthalmic Plastic & Cosmetic Surgery for Eyelid Cancer Reconstruction in St. Louis, MO?
Ophthalmic Plastic & Cosmetic Surgery offers exceptional expertise in eyelid cancer reconstruction in St. Louis, MO. Dr. John B. Holds, a fellowship-trained ophthalmic plastic surgeon, has been recognized in Best Doctors in America for decades and has authored more than 100 peer-reviewed publications on periocular reconstruction.
Dr. Holds is joined by Dr. Adam G. Buchanan, a fellowship-trained oculoplastic surgeon and former Army Colonel who serves as an examiner for the American Board of Ophthalmology, and Dr. Sara Reggie Giardina, who completed advanced oculofacial fellowships and focuses on individualized care. Together, their extensive surgical training and academic leadership deliver highly specialized reconstructive expertise.
FAQs
How Do I Know if I Need Reconstruction After Mohs Surgery on My Eyelid?
Most patients require some level of reconstruction after Mohs surgery because removing skin cancer often leaves a defect that cannot heal properly on its own — especially on the delicate eyelids. Small areas may sometimes be closed directly with stitches, but larger or deeper defects typically need specialized reconstruction to restore eyelid support, protect the eye, and maintain normal blinking.
If the removal affects the eyelid margin, tear duct, or deeper tissues, reconstruction becomes especially important. An oculofacial plastic surgeon evaluates the size, depth, and location of the defect to determine the safest and most functional repair approach.
Can Eyelid Cancer Reconstruction Be Performed on the Same Day as Cancer Removal?
Yes, reconstruction is often performed on the same day as cancer removal. In many cases, a Mohs surgeon removes the cancer first and confirms that all margins are clear. Once this is verified, reconstruction can begin immediately. This approach reduces the number of procedures and allows the eyelid to be repaired while the tissues are fresh. In some situations, cancer removal and reconstruction are performed in the same operating room using frozen section analysis to confirm complete excision.
What Happens if a Large Portion of My Eyelid Must Be Removed?
If a significant portion of the eyelid is removed, more advanced reconstructive techniques may be required. The eyelid plays a critical role in protecting and lubricating the eye, so rebuilding both its inner lining and outer structure is essential. Surgeons may use tissue from nearby areas, such as the upper eyelid or surrounding facial skin, to recreate natural support.
In certain cases, a staged procedure may be recommended to rebuild the eyelid in layers. The goal is to restore stable eyelid closure, maintain eye comfort, and achieve a natural appearance while protecting long-term vision.
Will Eyelid Reconstruction Affect My Vision Long Term?
When performed by a trained oculofacial plastic surgeon, eyelid reconstruction is designed to preserve and protect vision. The eyelids are essential for spreading tears, shielding the eye, and preventing dryness or irritation. Proper reconstruction restores these functions.
Temporary swelling or blurred vision may occur during early healing, but lasting vision problems are uncommon when the eyelid heals correctly. In fact, reconstruction often improves vision if cancer removal previously caused lid malposition or incomplete closure. Careful surgical planning focuses on maintaining eyelid alignment and protecting the cornea to support healthy, long-term visual function.
Are Skin Grafts or Flaps Ever Required for Eyelid Reconstruction?
Yes, skin grafts or local flaps are sometimes necessary, particularly when the surgical defect is too large to close directly. A skin graft involves transferring skin from another area, often behind the ear or from the upper eyelid, to cover the defect. A flap uses nearby tissue that remains attached to its blood supply and is repositioned to rebuild the eyelid.
The choice depends on the defect’s size, depth, and location. These techniques allow surgeons to restore eyelid contour, maintain proper support, and promote healing while preserving both function and appearance.
Schedule a Consultation for Eyelid Cancer Treatment in St. Louis
If you have already had skin cancer removed from your lids but want to improve function and appearance, or if you believe you have eyelid skin cancer, contact our office at (314) 567-3567 to discuss how we can help you to restore your health and look your best. We serve patients in St. Louis, St. Peters, and Arnold, MO.